Outdoor injury prevention is the one thing most active people think about only after something goes wrong and that timing is the entire problem. Every spring, as temperatures climb and athletes across New Jersey and New York return to trails, fields, and courts, orthopedic clinics see a predictable surge in injuries that were almost entirely avoidable.
At City Orthopaedics Sports Medicine, our specialists treat this wave every year across offices in East Rutherford, Paramus, West Orange, NJ. The patterns are consistent. So are the solutions.
Why Spring Is the Highest-Risk Season for Outdoor Sports Injuries
Spring injuries don’t happen because people are suddenly careless. They happen because of a specific physiological mismatch: your motivation is at 100%, but your body has been operating at 60% all winter.
During colder months, even active people reduce their volume, intensity, and movement variety. Muscles lose strength. Tendons lose elasticity. Neuromuscular coordination — your body’s ability to stabilize joints under load — quietly fades. Then the first warm weekend arrives, and most people try to pick up exactly where they left off in October. That gap between perceived fitness and actual readiness is the single biggest driver of spring sports injuries.
Knowing this changes how you approach the season. The goal isn’t to avoid activity — it’s to earn your way back into it.

Warm Up Smarter Static Stretching Before Activity Is a Mistake
Most people still warm up the wrong way. Holding a cold muscle in a static stretch doesn’t reduce injury risk — research shows it can actually reduce power output and increase strain risk in unprepared tissue.
The correct warm-up sequence for any outdoor activity:
- 5–10 minutes of light aerobic movement — a brisk walk, easy jog, or jumping jacks to raise core body temperature
- Dynamic stretching — leg swings, hip circles, walking lunges, high knees, and arm circles to mobilize joints through their full range
- Sport-specific priming — start tennis with easy groundstrokes, running at 60% effort, soccer with light passing drills
Save static stretching for your cool-down, when tissue is warm, pliable, and responding to lengthening. That’s when it genuinely improves flexibility.
The Most Common Outdoor Injuries and Exactly How to Prevent Each One
Knee Injuries
The knee is the most frequently injured joint in outdoor and spring sports — from runner’s knee and patellar tendonitis to ACL tears and meniscus damage. Injury rates peak in April and May when training loads spike fastest.
- Build quad and glute strength before the season — weak hips and thighs transfer excessive force to the knee
- Increase weekly mileage or session intensity by no more than 10% per week
- Avoid cutting and pivoting on wet, uneven, or unfamiliar surfaces until your body has adapted
- Replace athletic footwear that’s lost its cushioning — worn midsoles change how force travels through the knee
Dr. Oladapo M. Babatunde, MD, FAAOS, City Orthopaedics’ board-certified orthopedic surgeon and knee specialist, offers a clear rule of thumb: “Mild achiness after the first few outdoor workouts can be normal. But swelling, instability, or pain that doesn’t resolve within 48 to 72 hours is your signal to get evaluated — not to push through. Catching a knee problem early almost always means a faster, less invasive recovery.”
Foot and Ankle Injuries
Ankle sprains are the most common athletic injury across every outdoor sport. Plantar fasciitis, Achilles tendonitis, and stress fractures follow closely — especially when inactive feet are suddenly logging high miles on hard pavement.
- Inspect and replace your footwear before the season — shoes lose structural integrity after 300–500 miles even if they look fine externally
- Build ankle stability with single-leg balance drills and resistance band exercises
- Alternate between harder surfaces (road, turf) and softer ones (grass, trails) to reduce cumulative impact load
- Use ankle bracing or taping for high-risk activities if you have a prior sprain history
Dr. Jason Hymowitz, DPM, DABPM, AACFAS, MS, City Orthopaedics’ foot and ankle specialist, sees this pattern every spring without fail: “Dead shoes are one of the leading causes of plantar fasciitis and Achilles problems we treat. The outside of a shoe can look perfectly intact while the midsole has completely collapsed. If you’re starting the season in last year’s footwear, you may be starting it with a built-in injury risk.”
Shoulder and Upper Body Injuries
Throwing sports, tennis, cycling, and rowing bring shoulder and elbow injuries back into season every spring. Rotator cuff strains, shoulder impingement, and elbow tendonitis all share the same root cause — overhead and throwing load resumed too quickly after winter.
- Follow a structured interval throwing program before returning to full-effort throws
- Strengthen the rotator cuff and scapular stabilizers with targeted pre-season resistance work
- For racquet sports, check grip size and string tension — equipment mismatches are a direct cause of tennis and golfer’s elbow
Hydration: The Injury Factor Most Athletes Ignore
Dehydration isn’t just a heat issue — it directly affects injury risk. Muscle tissue that’s under-hydrated loses elasticity and fatigue resistance, making strains and cramps significantly more likely during spring outdoor activity, even on mild days.
- Drink water consistently throughout the day, not just during exercise
- For activity over 60 minutes, replenish electrolytes — water alone won’t replace sodium and potassium lost through sweat
- Watch for early dehydration signs: dry mouth, reduced urine output, unusual muscle cramping, or dizziness during exercise
- On warm spring days, start hydrating at least 2 hours before outdoor activity begins
Cross-Training: Your Best Defense Against Overuse
Repeating the same movements day after day — running the same route, playing the same sport — overloads specific muscle groups while underusing others. That imbalance is the foundation of overuse injuries like shin splints, stress fractures, and chronic tendonitis.
Rotate your training across different movement patterns: if you run three days a week, add a cycling or swimming day to offload the legs. If you play tennis regularly, add a strength training day focused on rotator cuff and wrist stability. Variety keeps your musculoskeletal system balanced and resilient throughout the full outdoor season.
The 10% Rule: Load Management Is Not Optional
The single most effective — and most ignored — principle in outdoor injury prevention is progressive load management. Your tendons, cartilage, and connective tissue adapt to stress more slowly than your cardiovascular fitness improves. You can feel in good shape while your joints are still lagging behind.
The rule is simple: never increase your weekly training volume — mileage, hours, or intensity — by more than 10% from one week to the next. This applies to every outdoor sport. It’s the difference between a season of progress and a season on the sidelines.
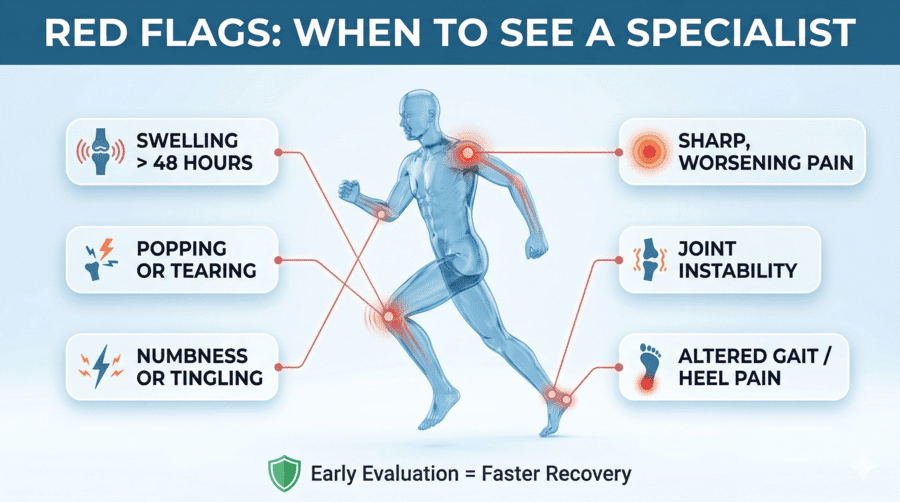
Red Flags: When to Stop and See a Specialist
Not everything needs immediate medical attention. But these symptoms do — and ignoring them converts small problems into big ones:
- Joint swelling that persists beyond 48 hours after activity
- Sharp, localized pain that worsens during — rather than improving through — activity
- A popping, snapping, or tearing sensation at the time of injury
- Knee or ankle instability — a feeling that the joint “gives out” under load
- Foot or heel pain that significantly alters your gait or running mechanics
- Numbness, tingling, or radiating pain in an arm or leg
These are not situations to manage with rest alone. Early evaluation at City Orthopaedics means faster diagnosis, more conservative treatment options, and a shorter path back to full outdoor activity.
Protect Your Season Before It Starts
The athletes who stay healthy all spring are the ones who prepare before the first run, the first game, or the first hike. Proper warm-up, smart load progression, the right footwear, cross-training, and hydration aren’t extra effort they’re the baseline for a full, injury-free outdoor season.
Whether you need a pre-season evaluation, have an existing injury that’s been nagging you, or want to understand your personal risk factors with an expert, Dr. Babatunde and Dr. Hymowitz are here for patients across East Rutherford, Paramus, and West Orange, NJ.
Start your season right not in a waiting room. Make outdoor injury prevention your first move this spring. Book an appointment at City Orthopaedics Sports Medicine today.
Frequently Asked Questions
What are the most common outdoor sports injuries in spring?
The most common spring outdoor injuries are ankle sprains, ACL and meniscus tears, runner’s knee, plantar fasciitis, Achilles tendonitis, rotator cuff strains, and stress fractures. Most occur because people return to full activity levels before their musculoskeletal system has adequately reconditioned after winter inactivity.
How much should I increase my training when starting outdoor activities in spring?
Follow the 10% rule — never increase your weekly training volume or intensity by more than 10% from one week to the next. This applies to mileage, session duration, and load. Progressing too quickly is the most common cause of overuse injuries like tendonitis and stress fractures in spring athletes.
Does dehydration increase the risk of sports injuries?
Yes. Dehydrated muscle tissue loses elasticity and fatigue resistance, raising the risk of strains, cramps, and coordination failures. Even on mild spring days, consistent hydration before, during, and after outdoor activity is an important injury prevention strategy — especially for sessions lasting over 60 minutes.
When should I see an orthopedic doctor for a spring sports injury?
Seek evaluation if you experience swelling that persists beyond 48 hours, sharp worsening pain during activity, a popping sensation at the time of injury, joint instability, or pain that changes your gait or movement mechanics. Early assessment leads to faster and less invasive treatment outcomes.
How do I know if my shoes are still good for spring outdoor activity?
Athletic shoes typically lose meaningful structural support after 300–500 miles of use, regardless of outward appearance. If your shoes are over a year old, show visible midsole compression, or feel less responsive than when new, replace them before starting your spring training season.
Where can I see a sports medicine specialist for spring or outdoor injury prevention in NJ or NY?
City Orthopaedics Sports Medicine has offices in East Rutherford, Paramus, and West Orange, NJ. Dr. Oladapo Babatunde (knee and sports medicine) and Dr. Jason Hymowitz (foot and ankle) see patients across all locations. Book your appointment here.