Plantar fasciitis is the most common cause of heel pain in adults and one of the most frustrating to live with. That first step out of bed in the morning, the stabbing pain after sitting too long, the ache that somehow gets worse after rest if any of this sounds familiar, you already know what plantar fasciitis feels like. What you may not know is what actually fixes it.
At City Orthopaedics Sports Medicine, our foot and ankle specialists treat plantar fasciitis patients every week across offices in East Rutherford, Paramus and West Orange, NJ. The condition is extremely common but the misinformation around it is even more common. This guide cuts through it.

What Is Plantar Fasciitis and Why Does It Hurt So Much?
The plantar fascia is a thick band of connective tissue that runs along the bottom of your foot, connecting your heel bone to your toes. It absorbs shock and supports the arch with every single step. When repetitive stress causes small micro-tears in this tissue, inflammation develops and that’s plantar fasciitis.
The signature symptom is sharp heel pain with the first steps of the morning or after prolonged rest. This happens because the fascia tightens while you’re off your feet, then is suddenly loaded when you stand. Pain often eases after a few minutes of walking but returns after long periods of standing, exercise, or hard surface impact.
Common risk factors include:
- Sudden increases in running mileage or training volume on hard surfaces
- Flat feet, high arches, or abnormal gait mechanics that strain the fascia unevenly
- Prolonged standing on hard floors common in healthcare workers, teachers, and retail staff
- Worn-out footwear that has lost its arch support and cushioning
- Tight calf muscles and a stiff Achilles tendon — the most consistently overlooked contributor
- Excess body weight increasing load concentration at the heel
What Actually Works for Plantar Fasciitis
The good news: the vast majority of plantar fasciitis cases resolve with non-surgical treatment. The frustrating reality: recovery requires time, consistency, and addressing the right things not just the symptoms.
Calf and Plantar Fascia Stretching
This is the single most evidence-backed intervention for plantar fasciitis. Tight calf muscles and a shortened Achilles tendon place constant excess tension on the plantar fascia, preventing it from healing. Stretching these structures multiple times daily especially before your first step in the morning consistently reduces pain and accelerates recovery.
- Plantar fascia-specific stretch: Sitting, cross one foot over the opposite knee, pull the toes back with your hand and hold 10 seconds perform 10 reps before getting out of bed each morning
- Towel/band calf stretch: Loop a towel around your foot, pull the toes toward you with the knee straight, hold 30 seconds repeat 3 times per side, twice daily
- Wall calf stretch: Both straight-knee and bent-knee variations to stretch the gastrocnemius and soleus muscles separately
Supportive Footwear and Orthotics
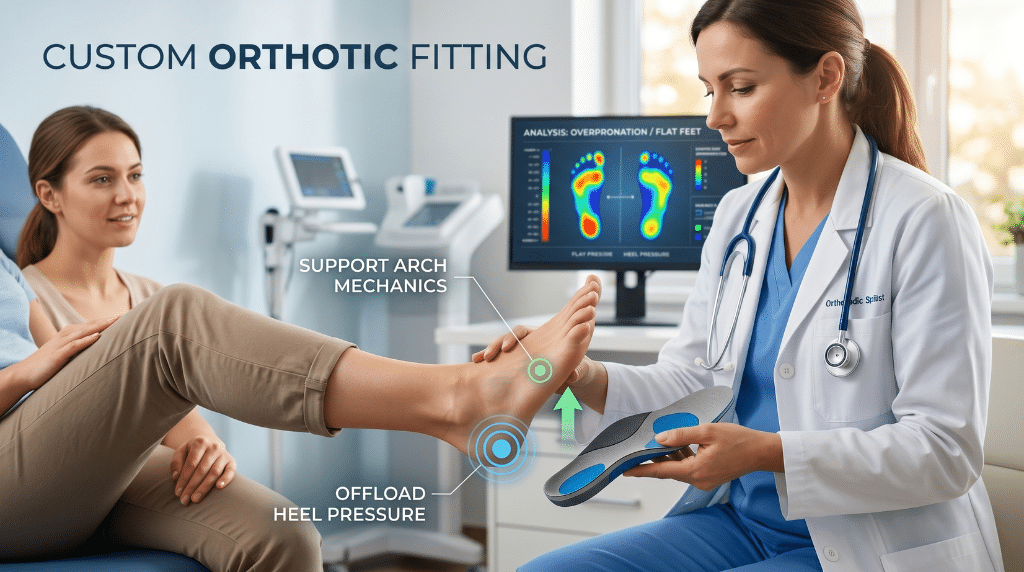
Replacing worn-out shoes is often the fastest single intervention for early-stage plantar fasciitis. Footwear should provide firm arch support, adequate heel cushioning, and a slight heel elevation. Walking barefoot on hard floors particularly first thing in the morning is one of the most aggravating habits a plantar fasciitis patient can have.
Custom or over-the-counter orthotics can offload pressure from the heel and support arch mechanics more precisely. For patients with structural contributors like flat feet or overpronation, properly fitted orthotics are a meaningful long-term tool not just temporary padding.
Night Splints
Night splints hold the foot in a gently dorsiflexed position during sleep, keeping the plantar fascia and calf muscles under a light stretch overnight. This eliminates the tightening cycle that causes that signature morning pain. Studies consistently show night splints reduce first-step pain in patients who use them regularly.
Physical Therapy
A structured PT program addresses the root causes of plantar fasciitis not just the symptoms. An effective protocol includes:
- Progressive calf and plantar fascia stretching program
- Intrinsic foot muscle strengthening — often called “foot core” training
- Gait analysis and correction for overpronation or abnormal heel-strike patterns
- Activity modification guidance that allows continued movement without reinjury
Ice and Anti-Inflammatory Measures
Icing the heel for 15–20 minutes after activity reduces acute inflammation effectively. Rolling the bottom of your foot over a frozen water bottle combines cryotherapy with self-massage of the fascia. Short-term NSAID use can manage pain during flare-ups — but it treats the symptom, not the mechanical cause, and should not be a long-term strategy.
What Doesn’t Work for Plantar Fasciitis
Knowing what to stop doing is just as important as knowing what to start.
- Complete rest alone: Total inactivity does not resolve plantar fasciitis. Without active stretching and loading progression, the tissue deconditions and becomes more vulnerable. Low-impact activity like swimming and cycling is encouraged throughout recovery.
- Continuing in worn-out shoes: No amount of stretching compensates for a collapsed arch underfoot. Footwear evaluation is non-negotiable in any plantar fasciitis treatment plan.
- Expecting quick results: Most cases take 6–18 months to fully resolve. Patients who abandon treatment after 2–3 weeks because they “didn’t see improvement fast enough” are the ones who end up in chronic, recurring pain.
- Ignoring tight calves: If Achilles and calf flexibility isn’t addressed, every other treatment becomes significantly less effective. This is the most commonly missed step.
- Relying solely on cortisone injections: Injections are a valuable adjunct not a standalone fix. Multiple injections without addressing the underlying mechanics can weaken plantar fascia tissue over time.
When to Stop Self-Treating and See a Specialist
Home management is appropriate for most early-stage cases. But these are clear signals that it’s time for a professional evaluation:
- Pain has persisted for more than 6–8 weeks despite consistent stretching and footwear changes
- Pain is severe enough to alter how you walk or significantly restrict daily activity
- Symptoms are worsening rather than gradually improving with self-care
- Pain is located along the arch or midfoot not just the heel which may point to a different diagnosis
- You’ve had multiple recurrences and want to address the root mechanical cause permanently
Dr. Jason Hymowitz, DPM, DABPM, AACFAS, MS, City Orthopaedic’s foot and ankle specialist, sees plantar fasciitis cases across the full severity spectrum.
“The patients who struggle most are usually the ones who waited too long,” says Dr. Hymowitz.
“By the time they come in, they’ve developed compensatory movement patterns, sometimes a secondary Achilles issue, and the fascia is in a chronic degenerative state rather than acute inflammation. Earlier evaluation means faster, simpler treatment and a much shorter recovery.”

Advanced Plantar Fasciitis Treatments When Conservative Care Isn’t Enough
When a genuine trial of conservative care typically 8–12 weeks of consistent PT, stretching, and footwear correction hasn’t provided adequate relief, more advanced options are available at City Orthopaedics:
- Corticosteroid injections: Ultrasound-guided cortisone injections deliver targeted anti-inflammatory medication directly to the point of maximal tenderness — effective for short-to-medium-term relief, especially alongside PT
- Platelet-Rich Plasma (PRP): Growth factors from the patient’s own blood are concentrated and injected into the damaged fascia to stimulate healing increasingly preferred for chronic cases where tissue degeneration has set in
- Extracorporeal Shock Wave Therapy (ESWT): A non-invasive procedure delivering focused sound waves to the heel to stimulate tissue repair well-supported in clinical literature for refractory plantar fasciitis
- Surgical plantar fascia release: Reserved only for truly refractory cases after 12+ months of failed conservative treatment rarely needed, but available when all other options have been exhausted
Don’t Let Heel Pain Become a Chronic Condition
Most people with plantar fasciitis recover fully but only when they address the right factors consistently and get expert guidance before the condition becomes entrenched. Left unmanaged, plantar fasciitis alters gait mechanics, strains the Achilles and knee, and significantly limits activity and quality of life for months to years.
City Orthopaedics Sports Medicine offers comprehensive foot and ankle care at offices across East Rutherford, Paramus, and West Orange, NJ. From your first evaluation through advanced treatment and full return to activity, our team has the expertise to get you back on your feet pain-free.
Book an appointment at City Orthopaedics Sports Medicine today and get a personalized plantar fasciitis treatment plan from a specialist who understands your foot and your goals.
Frequently Asked Questions About Plantar Fasciitis
How long does plantar fasciitis take to heal?
Most plantar fasciitis cases resolve within 6–18 months with consistent conservative care. Patients who stretch diligently, address footwear, and complete a structured PT program typically see meaningful improvement within the first 6–8 weeks. Chronic cases left untreated for extended periods often take longer and may require advanced intervention.
What is the single best stretch for plantar fasciitis?
The plantar fascia-specific stretch pulling the toes back before your very first morning step is the most consistently effective single exercise. Performed before getting out of bed, it pre-stretches the fascia and significantly reduces that characteristic first-step pain. Pair it with calf and Achilles stretching throughout the day for best results.
Should I stop running if I have plantar fasciitis?
Not necessarily. Complete rest is rarely required and often counterproductive. Reducing mileage, switching to softer surfaces, upgrading footwear and orthotics, and avoiding speed or hill work during a flare typically allows gradual continuation of running while the fascia heals. A specialist can guide sport-specific activity modification for your case.
Are cortisone injections safe for plantar fasciitis?
Cortisone injections are a safe and effective short-term tool when used appropriately. However, repeated injections can weaken the fascia tissue over time, increasing rupture risk. They work best as a complement to stretching and PT not as a standalone solution. Most physicians limit injections to two or three per treatment course.
What is the difference between plantar fasciitis and a heel spur?
A heel spur is a bony growth on the underside of the heel bone, often visible on X-ray. Many people with heel spurs have zero symptoms, while many plantar fasciitis patients have no spur at all on imaging. Plantar fasciitis pain comes from tissue inflammation not the spur itself meaning treatment targets the fascia regardless of whether a spur is present.
Where can I see a foot specialist for plantar fasciitis in New Jersey or New York?
City Orthopaedics Sports Medicine offers expert plantar fasciitis evaluation and treatment at offices in East Rutherford, Paramus, and West Orange, NJ, and Manhattan, NY. Dr. Jason Hymowitz, DPM, DABPM, AACFAS, MS, leads foot and ankle care across all locations. Book your appointment here.